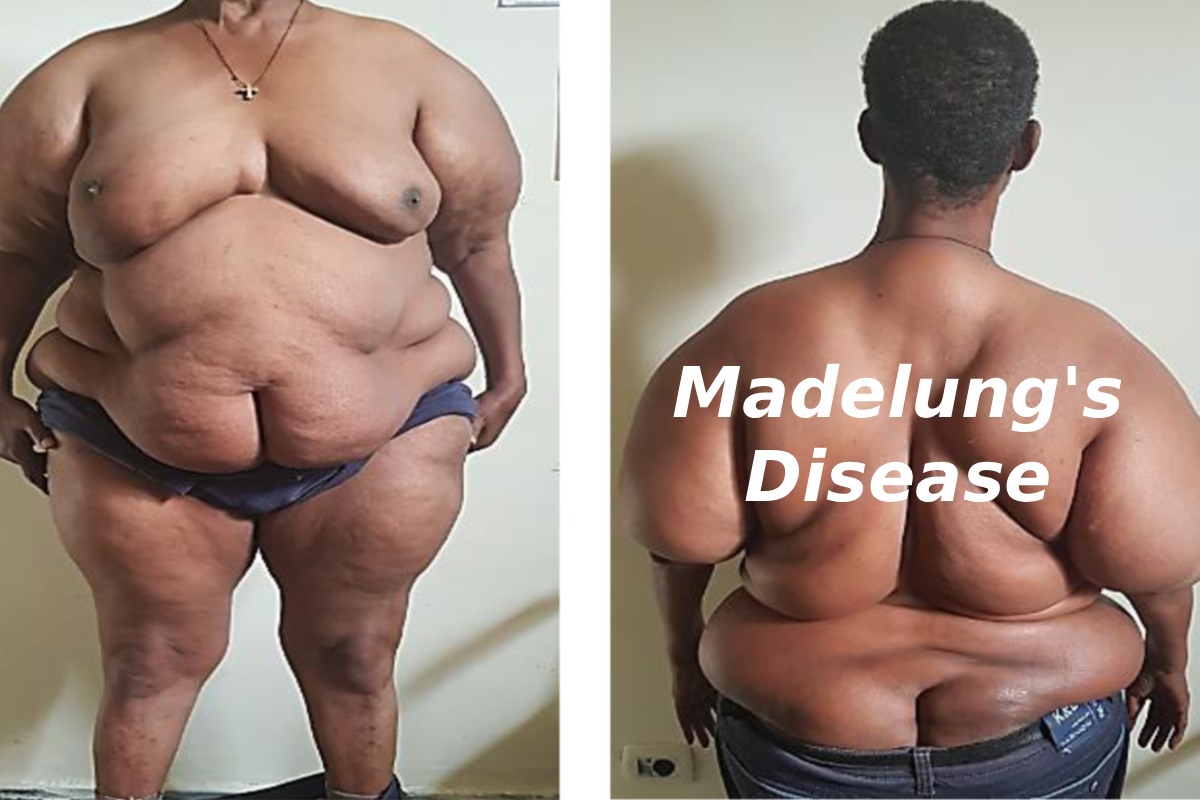
Madelung’s Disease—also called Multiple Symmetric Lipomatosis (MSL)—is a rare metabolic disorder where non-cancerous fat masses grow symmetrically, mainly around the neck, shoulders, upper arms, and upper chest. It’s uncommon, often misunderstood, and very distinctive in how it looks and behaves.
Table of Contents
What is Madelung’s Disease?
Madelung’s Disease is a rare medical disorder characterized by the abnormal, symmetric buildup of fatty tissue (lipomas), characteristically near the neckline, shoulder joints, upper arms, and upper chest. It is also called Manifold Symmetric Lipomatosis (MSL).
Unlike ordinary obesity, the fat deposits in Madelung’s Disease are non-encapsulated, effortless, and generous, often causing cosmetic concerns or, in plain cases, functional problems such as limited neck movement or compression of nearby structures.
Here’s a concise overview of Madelung’s Disease in table form:
| Aspect | Details |
| Names | Multiple Symmetric Lipomatosis (MSL) |
| Meaning | Rare illness causing abnormal, symmetric accumulation of fatty tissue, typically in the neck, shoulders, upper arms, and trunk. |
| Causes / Risk Factors | Genetic predisposition, chronic alcohol use, mitochondrial dysfunction, metabolic disorders, and male gender. |
| Symptoms | Symmetric fatty deposits, limited mobility, beautifying concerns, heaviness, compression symptoms, metabolic or neurological issues. |
| Diagnosis | Physical inspection, medical history, imaging (CT/MRI/ultrasound), lab tests, differential diagnosis. |
| Treatment | Medical excision, liposuction, lifestyle changes (alcohol cessation), indicative medical therapy, and regular monitoring. |
| Problems | Nerve density, airway obstruction, limited mobility, cosmetic/psychological impact, metabolic disorders, and reappearance after surgery. |
| Prognosis | Chronic condition; surgical removal improves function/arrival, but recurrence is possible. |
| Populace Pretentious | Mostly middle-aged men; less common in women. |
| Key Thought | Early diagnosis and intervention can help reduce developmental delays. |
What Causes Madelung’s Disease?
Here’s a clear table showing the causes of Madelung’s Disease:
| Cause / Risk Factor | Description |
| Genetic Predisposition | It may run in relatives; in some cases, it shows autosomal dominant inheritance. |
| Chronic Alcohol Ingestion | Strongly related, alcohol may trigger abnormal fat metabolism. |
| Mitochondrial Dysfunction | Reduced energy production in cells may lead to irregular fat deposition. |
| Metabolic Diseases | Conditions such as insulin resistance, liver disease, or abnormal lipid metabolism can contribute. |
| Male Gender | More common in middle-aged men than in women. |
| Unknown / Idiopathic Factors | In some cases, no clear cause is documented. |
What Are the Common Symptoms of Madelung’s Disease?
Here’s a clear table showing the common symptoms of Madelung’s Disease:
| Symptom | Description |
| Symmetrical Fatty Deposits | Effortless, slow-growing fat masses around the neck, shoulders, upper arms, and trunk. |
| Limited Mobility | Large deposits may restrict neckline or arm movement. |
| Cosmetic Anxieties | Visible swelling can affect arrival and self-confidence. |
| Neck or Upper Body Heaviness | Feeling of weight or bulkiness in affected areas. |
| Density Symptoms | Rarely, large masses can bandage nerves or the airway, causing discomfort. |
| Metabolic or Nervous Symptoms | Occasionally associated with liver problems, neuropathy, or metabolic issues. |
What Autoimmune Disease Causes Lipomas?
Here’s a table showing autoimmune and related circumstances that can cause lipomas:
| Autoimmune / Related Disease | Description / How it Causes Lipomas |
| Familial Multiple Lipomatosis (FML) | A genetic disorder is sometimes associated with immune dysregulation, leading to multiple lipomas. |
| Proteus Syndrome | A rare disorder characterized by irregular tissue growth, including lipomas, and involving the immune system. |
| Madelung’s Disease (Multiple Symmetrical Lipomatosis) | Not strictly autoimmune, but metabolic and mitochondrial dysfunction may have immune components, causing symmetric lipomas. |
| Autoimmune Thyroid Disease (Hashimoto’s, Graves’) | Rarely linked to subcutaneous lipomas, possibly due to metabolic changes and inflammation. |
| Dercum’s Disease (Adiposis Dolorosa) | Chronic, painful lipomas are associated with inflammatory and autoimmune conditions. |
How is Madelung’s Disease Diagnosed?
Here’s a clear table showing how Madelung’s Disease is diagnosed:
| Analytic Method | Description |
| Physical Inspection | Initial valuation of regular, painless fat deposits and their distribution. |
| Medical History | Evaluates alcohol use, family history, and onset of indications. |
| Imaging Education (CT / MRI) | Determines the size, extent, and depth of fat deposits and helps distinguish them from other conditions. |
| Ultrasound | It can be used to assess superficial lipomas and tissue characteristics. |
| Workroom Tests | May check for liver function, lipid levels, and metabolic disorders. |
| Differential Diagnosis | Rules out other conditions such as obesity, Cushing’s syndrome, or solitary lipomas. |
What Treatments Are Available for Madelung’s Disease?
Here’s a clear table presentation of the treatment options for Madelung’s Disease:
| Treatment | Description / Purpose |
| Surgical Editing | Direct removal of fatty masses; used for cosmetic or useful reasons. |
| Suction lipectomy | Minimally aggressive method to reduce large fatty deposits and improve appearance. |
| Lifestyle Changes | Alcohol cessation and a healthy diet may slow disease development. |
| Medical Therapy (Limited) | No definitive drug treatment; sometimes, indicative medications are used for pain or metabolic issues. |
| Regular Nursing | Follow up to track deposit growth and check for complications. |
| Organization of Problems | Treats nerve compression, breathing issues, or metabolic disorders if they arise. |
Types of Madelung’s Disease
Here’s a clean, easy-to-understand table of the types of Madelung’s Disease (Multiple Symmetric Lipomatosis):
| Type | Alternate Name | Pattern of Fat Distribution | Common Areas Affected | Typical Appearance | Key Notes |
| Type I | Cervical Type | Localized, well-defined symmetric fat masses | Neck, nape, shoulders, upper back | “Horse-collar” neck, bulky upper torso | Most common; may cause breathing or swallowing difficulty |
| Type II | Pseudo-obese Type | Diffuse, symmetric fat accumulation | Upper arms, chest, abdomen, thighs | Looks like generalized obesity | Hard to distinguish from obesity; fat does not reduce with weight loss |
| Type III | Gynecoid Type (Rare) | Predominantly lower-body fat deposition | Hips, buttocks, thighs | Pear-shaped body | Very rare; more common in women |
| Type IV | Mixed Type (Very Rare) | Combination of localized and diffuse patterns | Upper and lower body | Irregular but symmetric fat growth | Shares features of multiple types |
Prices in India, UK, USA, and London Madelung’s Disease
Here’s a projected comparison of treatment costs for Madelung’s Disease (fatty mass removal/lipoma surgery) in India, the UK (including London), and the USA. Note that Madelung’s Disease surgery often involves removing multiple symmetric fatty deposits, so actual costs can vary widely based on the number, size, complexity, hospital choice, and whether the insurance covers part of the cost. These are estimated ranges based on obtainable data for lipoma/fatty lump removal, which is similar to parts of Madelung’s surgical organization.
| Country | Typical Price Range (approx.) | Notes |
| India | ₹15,000 – ₹1,00,000+ per area / lipoma | The cost of surgical excision or lipoma elimination varies widely by city, surgeon, and lesion size. Some clinics bundle manifold removals into packages. |
| UK | £300 – £1,500+ per lipoma | Private lipoma removal in the UK typically falls in this range; larger or deeper masses can cost more. |
| London (UK) | £350 – £1,500+ per lipoma | London often sits at the upper end of UK valuing due to higher facility and doctor costs. |
| USA | ~$2,000 – $4,000+ per lipoma | The average lipoma removal cost in the US is around $3,000, but this can vary by clinic and complexity. |
A Non–Alcohol-Related Case of Madelung’s Disease
Here’s a table brief on a non–alcohol-related case of Madelung’s Disease:
| Aspect | Details |
| Patient Profile | Middle-aged male, no history of alcohol ingestion. |
| Symptoms | Symmetric, painless fatty deposits on neck and shoulders; mild discomfort. |
| Medical History | No metabolic illnesses; family history negative for lipomatosis. |
| Cause / Risk Factor | Likely genetic predisposition or mitochondrial dysfunction. |
| Diagnosis | Physical examination and MRI confirmed multiple symmetric lipomas. |
| Treatment | Surgical excision of the largest crowds; lifestyle maintained. |
| Outcome / Forecast | Improved appearance and mobility; low recurrence at 1-year follow-up. |
| Key Point | Madelung’s Disease can occur without alcohol use, highlighting genetic/metabolic factors. |
What Complications Can Arise from Madelung’s Disease?
Here’s a clear table showing the possible complications of Madelung’s Disease:
| Complication | Description |
| Compression of Nerves | Large fatty deposits may press on nerves, causing pain, numbness, or weakness in the affected areas. |
| Airway Barrier | Fat accumulation around the neck can restrict breathing in severe cases. |
| Limited Mobility | Excess fat around the neck, shoulders, or arms may reduce the range of motion. |
| Improving / Psychological Impact | Visible fat masses can lead to self-consciousness, stress, or unhappiness. |
| Metabolic Disorders | Occasionally associated with insulin resistance, liver disease, or dyslipidemia. |
| Recurrence After Surgery | Even after removal, fatty deposits may regrow over time, requiring further treatment. |
Conclusion
Madelung’s Disease, or Multiple Symmetric Lipomatosis, is a rare illness characterized by abnormal, symmetric fat accumulation in the neck, shoulder joint, upper arms, and trunk. While the careful reason is not fully tacit, genetic factors and chronic alcohol use are involved. Mitochondrial dysfunction is also a key contributor.
FAQS
What is Madelung’s Disease?
A rare disorder causing symmetrical, painless fat deposits around the neck, shoulder joint, and upper body.
What are the reasons for Madelung’s Disease?
Genetic issues, lingering alcohol use, and metabolic or mitochondrial dysfunction.
What are the symptoms?
Symmetric greasy masses, incomplete mobility, weight, and cosmetic concerns.
How is it identified?
Through physical review, imaging (CT/MRI), and medical history.
How is it preserved?
Medical removal, liposuction, lifestyle changes, and indicative management.
Can it come back after treatment?
Yes, fatty deposits can recur, necessitating further management.
Who is most pretentious?
Typically, middle-aged men, chiefly those with a history of alcohol use.
Are there problems?
Yes, including nerve compression, airway obstruction, and mobility limitations.
Is there a treatment?
No, action manages signs and improves influx/purpose, but does not prevent reappearance.
Can lifestyle changes help?
Yes, alcohol cessation and healthy habits may slow progression.