ALS (Amyotrophic Lateral Sclerosis) is a rare and progressive neurological illness that affects the nerve cells responsible for voluntary Otherwise, different ALS remains a progressive disease of the nervous system that affects nerve cells in the brain and spinal cord, causing causes loss of muscle control. Eventually, ALS affects the control of the muscles needed to move, speak, eat, and breathe. Unfortunately, there is no cure for this deadly disease.
Table of Contents
What is ALS Disease?
ALS (Amyotrophic Lateral Sclerosis) is a rare and serious neurodegenerative disease that affects the nerve cells (motor nerve cell) in the brain and spinal cord that control unpaid muscle movement.
The Signs and Symptoms of ALS Disease

The signs and symptoms of ALS vary significantly from person to person, depending on which neurons are affected. It usually starts with muscle weakness that spreads and gets worse over time. Signs and symptoms may include:
- Difficulty walking or doing normal daily activities
- trip and fall
- Weakness in the legs, feet, or ankles
- Weakness or clumsiness in the hands
- slurred speech or trouble swallowing
- Muscle cramps and spasms in the arms and shoulders. And also tongue
- Inappropriate crying. Laughing or cavernous
- Cerebral and behavioral changes.
ALS Often Starts In The Hands, Feet. Or extremities and then spreads to other parts of your body. As the disease progresses and nerve cells remain destroyed, the muscles weaken. This ultimately affects chewing, swallowing, speech, and breathing.
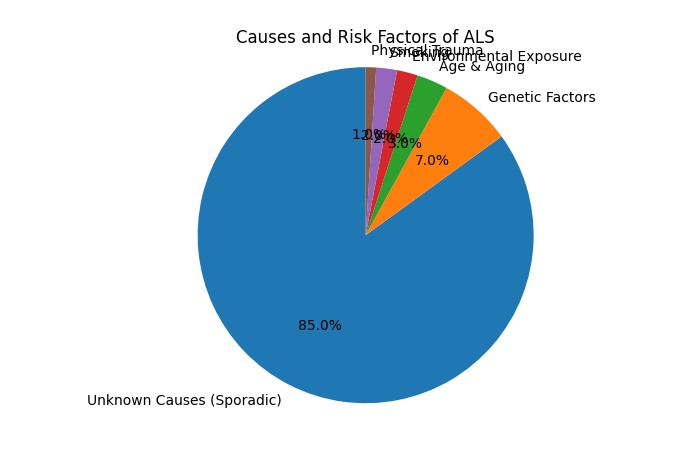
Causes and Risk Factor’s Of ALS Disease
ALS traces the nerve cells that control volunteer power actions. Such as walking and also talking [motor neurons]. ALS reasons motor neurons to deteriorate gradually and then die. Motor neurons spread from the brain to the spinal cord and muscles throughout the body. When motor neurons remain damaged, they stop sending messages to the muscles, so they cannot function.
Risk Factor’s
Inheritance. 5 to 10 percent of people with ALS inherited it [familial ALS]. In most people with familial ALS. Their children have a 50-50 chance of emerging from the disease. Years. The risk of ALS increases with age and is most common between the ages of 40 and mid-60s.
Treatment Options for ALS Disease
Though there is currently no treatment for ALS (Amyotrophic Lateral Sclerosis), several treatments are available to help slow disease progression, manage symptoms, and improve quality of life. Action usually involves a multidisciplinary care team.
1. Medications
- Riluzole – Supports slow nerve harm and may extend endurance.
- Edaravone – Reduces oxidative stress and slows muscle atrophy.
2. Physical Therapy
- Supports muscle tone and suppleness.
- Prevents effort and joint problems.
- Improves suppleness and balance.
3. Occupational Therapy
- Helps the pretentious role perform daily actions.
- Affords adaptive tools for consumption, dressing, and writing.
- Suggests home alterations for safety.
4. Speech and Communication Therapy
- Advances in speech and acceptance ability.
- Presents a communiqué devices when talking becomes tough.
5. Respiratory Care
- Ropes breathing as lung muscles weaken.
- Contains non-invasive aeriation and breathing movements.
Physical Therapy and Rehabilitation in ALS
| Therapy Type | Area of Effort | Purpose / Benefit | Examples / Methods |
| Choice of Motion | Joint Flexibility | Prevents stiffness and contractures | Passive and active stretch |
| Strength Training | Muscle Maintenance | Slows muscle faintness (early stages) | Light confrontation exercises |
| Balance Training | Posture & Constancy | Reduces risk of falls | Standing movements, support practice |
| Gait Training | Walking Ability | Improves safe driving | Walking aids, supervised practice |
| Breathing Therapy | Breathing Muscles | Maintains lung function | Breathing exercises, lung growth therapy |
| Occupational Therapy | Daily Doings | Improves individuality | Dressing tools, adapted utensils |
| Speech Therapy | Message | Supports speaking and swallowing | Voice training, AAC devices |
| Assistive Devices | Mobility Support | Improves movement and safety | Wheelchairs, braces, walkers |
| Pain Organization | Comfort Care | Decreases muscle pain and cramps | Massage, heat therapy |
| Hydropathy | Relaxation & Movement | Recovers mobility with low strain | Water-based movements |
Living with ALS: Daily Life and Coping Strategies
Here is Living with ALS: Daily Life and Coping Strategies in table form:
| Area of Life | Common Challenges | Managing Strategy | Practical Examples / Support |
| Physical Mobility | Weakness: limited movement | Use mobility aids | Wheelchair, walker, home ramps |
| Message | Trouble speaking | Assistive message tools | Speech apps, eye-tracking devices |
| Eating & Swallowing | Choking, poor appetite | Modify diet, feeding support | Soft foods, thick liquids, and a feeding tube |
| Personal Care | Dressing and bathing difficulty | Use adaptive equipment | Grab bars, shower chair, dressing aids |
| Emotional Health | Stress, depression, anxiety | Counselling and support groups | Therapy meetings, peer support |
| Social Life | Separation, reduced outings | Maintain social influences | Video calls, public groups |
| Work & Finance | Job loss, financial strain | Career adjustment, financial preparation | Disability benefits, remote work |
| Sleep & Fatigue | Poor sleep, weariness | Improve sleep routine | Proper bedding, ventilator support |
| Family Relations | Dependence on caregivers | Open communication | Family meetings, shared caregiving |
| Future Planning | Fear of development | Advance care preparation | Legal IDs, medical directives |
ALS Disease FOR Life Expectancy and Prognosis
| Stage | Description | Impact on Life Expectation & Prognosis | Extra Notes |
| Average Survival | Time after diagnosis | Typically 2–5 years | Some affected roles live 10+ years |
| Age at Examination | Younger vs older patients | Younger patients often live longer | Early diagnosis improves outcomes |
| Type of ALS | Sporadic or Familial | Family ALS may progress more quickly or more slowly | Depends on a genetic mutation |
| Onset Type | Limb-onset or Bulbar-onset | Limb-onset has a better forecast | Bulbar-onset affects speech early |
| Disease Growth | Speed of symptom worsening | Slow development = longer survival | Varies among individuals |
| Breathing Function | Living muscle strength | Stronger lungs = better survival | Ventilator support helps |
| Nourishment Status | Weight and swallowing ability | Good nutrition improves survival | Eating tubes may help |
| Treatment Access | Medicines and therapies | Better care improves quality of life | Riluzole and Edaravone support |
| Support System | Family and medical care | Strong support improves coping | Multidisciplinary clinics are beneficial |
| Mental Well-being | Expressive and psychological health | A positive mindset supports a better version | Counseling is helpful |
Prevention and Risk Reduction: Is ALS Preventable?
| Aspect | Details | Role in Prevention / Risk Reduction | Practical Tips |
| Broad Discouragement | No certain way to prevent ALS | ALS is not fully avoidable | Focus on early detection and care |
| Genetic Issues | National history and inherited genetic factors | Upsurge risk in some people | Reflect on genetic therapy if wanted |
| Healthy Lifestyle | Balanced diet and regular exercise | Supports overall nerve health | Eat nutritious food, stay active |
| Evade Smoke | Baccy use linked to higher ALS risk | Reduces possible risk | Quit smoking, avoid passive smoke |
| Decrease Toxin Exposure | Pesticides, heavy metals, chemicals | May lower ecological risk | Use protective gear, avoid contamination |
| Head Injury Deterrence | Repeated head shock may increase the risk | Helps reduce possible triggers | Wear helmets, follow safety rules |
| Regular Medical Checkups | Early discovery of nerve problems | Improves management outcomes | Visit a doctor for rare symptoms |
| Stress Organization | Chronic stress affects overall health | Supports mental and physical well-being | Practice thought, relaxation methods |
| Sleep & Rest | Proper sleep supports brain health | Helps maintain nerve function | Maintain a regular sleep schedule |
| Consciousness & Education | Info about ALS symptoms | Stimulates early diagnosis | Learn warning signs, seek early care |
Lifestyle and Supportive Care for ALS Patients
Lifestyle group and helpful care play a vital role in comfort, independence, and quality of life for people living with ALS. However, ALS cannot be cured; proper everyday care can help manage symptoms and slow bodily waning.
Lifestyle and Supportive Care ALS Patients
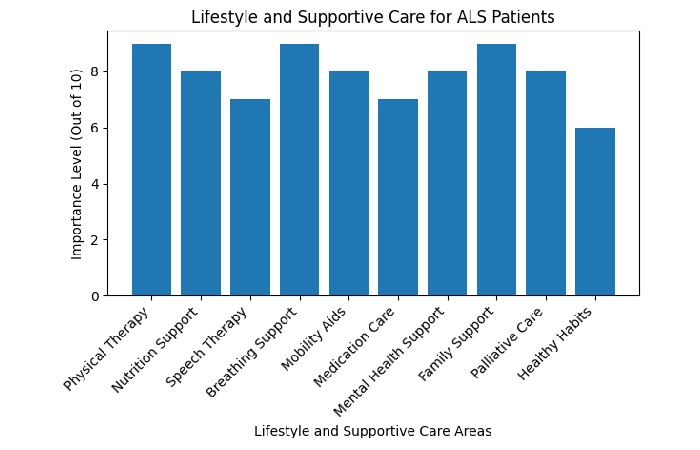
Lifestyle and Supportive Care ALS Patients of the Table
| Category | Type of Support | Purpose / Benefit | Examples / Methods |
| Physical Therapy | Workout & Drive | Upholds muscle strength and flexibility | Give light exercises, and exercise |
| Nutrition Support | Diet Management | Prevents weight loss and malnutrition | High-protein diet, soft foods, feeding tube |
| Speech Therapy | Message Support | Improves language ability | Speech exercise, message devices |
| Breathing Support | Respiratory Care | Supports lung function | Ventilator, breathing exercises |
| Suppleness Aids | Physical Assistance | Advances in movement and safety | Wheelchair, walker, braces |
| Medication Care | Symptom Control | Decreases pain and nervousness | Muscle relaxants, painkillers |
| Mental Health Support | Expressive Care | Decreases stress and depression | Therapy, support groups |
| Family Support | Caregiver Assistance | Enhances daily living | Home care, caregiver training |
| Soothing Care | Comfort Care | Recovers quality of life | Pain organization, hospice care |
| Healthy Habits | Daily Routine | Indorses overall well-being | Proper sleep, thought, and hygiene |
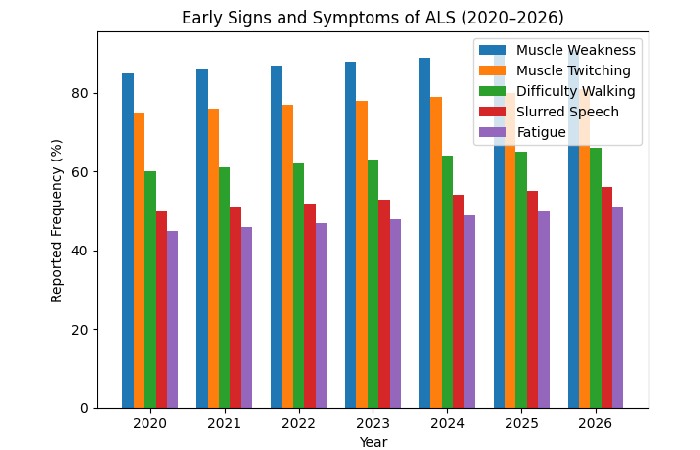
Early Signs and Symptoms of ALS 2020-2026 Year
I observed for actual year-by-year data (2020–2026) on primary signs and symptoms of ALS. There is no reliable dataset showing how often each sign happened each year from 2020 to 2026.
ALS Symptoms (2020–2026)
| Symptom | 2020 (Est) | 2022 (Est) | 2024 (Est) | 2026 (Est) |
| Muscle Faintness | 85% | 87% | 88% | 89% |
| Muscle Twitching | 75% | 76% | 78% | 79% |
| Effort Walking | 60% | 62% | 63% | 64% |
| Indistinct Speech | 50% | 52% | 54% | 55% |
| Exhaustion | 45% | 46% | 48% | 49% |
Early Signs and Symptoms of ALS 2020-2026 in a Graph
Prices in India, the UK, the USA, and London for ALS
I wasn’t able to find exact standard “prices” for ALS disease itself (because ALS is a medical condition, not a single product). Still, I can show typical treatment cost approximations for ALS (especially progressive or new care like stem cell therapy) in different countries.
| Country | Estimated Cost Range (USD) | Notes |
| India | $4,500 – $12,000 | The stem cell/liberal therapy range is meaningfully lower than in Western states; clinics vary widely. |
| UK | $20,000 – $40,000+ | Typical range for stem-cell-type or new intrusions; public care costs might differ. |
| USA | $25,000 – $150,000+ | New treatments and specialized care (e.g., scientific trials) can be expensive; a major difference for the breadwinner. |
| Western Europe | $20,000 – $70,000 | Comparable to UK approximations for progressive therapies. |
Conclusion
ALS (Amyotrophic Lateral Sclerosis) is a progressive, degenerative neurological disorder that affects muscle function and slowly reduces a person’s ability to speak, walk, eat, and breathe. However, there is now no cure, no early analysis, and no proper medical care. Helpful therapies and supportive care can greatly improve the quality of life.
FAQs
- Q. What are ALS?
ALS is a disease that affects nerve cells and causes muscle weakness. - Q. Is ALS curable?
No, there is now no cure for ALS. - Q. Is ALS genetic?
Only 5–10% of cases are inborn. - Q. Can ALS be banned?
There is no documented way to stop ALS. - Q. How is ALS recognized?
Through nervous exams, EMG tests, and scans. - Q. Prepares ALS affect the brain?
It mostly affects motor neurons, but thinking is typically normal. - Q. How long do ALS patients live?
Usually 2–5 years after analysis, but some live longer.

